What is Bipolar Disorder?
Bipolar disorder, also known in some parts of the world by its older name, “manic depression,” is a mental disorder that is characterized by serious and significant mood swings. A person with this condition experiences alternating “highs” (what clinicians call “mania“) and “lows” (also known as depression).
Both the manic and depressive periods can be brief, from just a few hours to a few days. Or the cycles can be much longer, lasting up to several weeks or even months. The periods of mania and depression vary from person to person — many people may only experience very brief periods of these intense moods, and may not even be aware that they have the disorder.
According to the American Psychiatric Association, there four major categories of bipolar disorder: bipolar I disorder, bipolar II disorder, cyclothymic disorder, and bipolar disorder due to another medical or substance abuse disorder (APA, 2013). Anyone can be diagnosed with bipolar disorder, but bipolar disorder in children is called disruptive mood dysregulation disorder and is characterized by a different set of symptoms.
All types of bipolar disorder generally respond well to treatment, which usually includes medication management for many years and for some, psychotherapy. Like many mental disorders, professionals generally don’t talk about a person being “cured” of this condition, so much as learning to manage it well. Medication and psychotherapy help a person do that.
Learn more: Frequently Asked Questions & Fact Sheet
Symptoms of Bipolar
For bipolar disorder to be diagnosed, a person needs to have experienced at least one manic (or in bipolar II, hypomanic) episode, and one depressive episode during their lifetime.
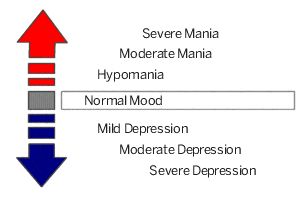
A manic episode (bipolar I disorder) is characterized by extreme happiness, extreme irritability, hyperactivity, little need for sleep and/or racing thoughts, which may lead to rapid speech. People in a manic episode feel like they can do anything, make plans to try and do all those things, and believe that nothing can stop them. For bipolar I to be diagnosed, this episode must have last at least a week and represents a noticeable change from a person’s usual behavior.
A hypomanic episode (bipolar II disorder) is characterized by the same symptoms as a manic episode, except the symptoms need to only have been present for at least four (4) days.
A depressive episode is characterized by extreme sadness, a lack of energy or interest in things, an inability to enjoy normally pleasurable activities and feelings of helplessness and hopelessness. On average, someone with this condition may have up to three years of normal mood between episodes of mania or depression.
When left untreated, the severity of episodes can vary. People with this condition can often predict when a new cycle is starting, as the severity of their symptoms increase.
Learn more: Review the complete symptoms of bipolar disorder.
Causes & Diagnosis
As with most mental disorders, researchers are still not certain what causes this condition. There is no single risk factor, gene, or other predisposition that puts a person at increased risk for bipolar disorder. It is likely a combination of factors increase a person’s risk. According to research, these factors may include a different brain structure and way of functioning, a set of genetic factors, and family history (as this disorder tends to run in families).
Learn more: What are the Causes of Bipolar Disorder?
Bipolar disorder, like most mental disorders, is best diagnosed by a trained mental health professional — such as a psychologist, psychiatrist, or clinical social worker. While a family physician or general practitioner may offer a preliminary diagnosis, only a mental health specialist offers the experience and skills necessary to diagnose this condition reliably.
Learn more: How is Bipolar Diagnosed?
Bipolar Disorder Treatment
According to researchers at the National Institute of Mental Health (NIMH), the exact cause of bipolar disorder is not yet known. Despite this limitation, the disorder can still be effectively treated. Research into the most effective treatments is ongoing.
Like most mental disorders, today this condition is treated with psychotherapy combined with psychiatric medications (most people benefit more quickly from combined treatment of the two). Treatment for this disorder is generally effective and helps most people keep a balanced mood throughout their day, most days of the month. It may take anywhere from one to two months before a person starts feeling the full, beneficial impact of their treatment.
Self-help strategies for this condition vary in their effectiveness, depending upon the person and the severity of the disorder. Some people find it beneficial to join a support group, read books explaining effective self-help strategies, or keeping a journal (either paper or through a mood or journaling app).
One of the biggest challenges of treatment of bipolar disorder is finding and maintaining a treatment routine that works best for a person over the long-term. Most people with this condition benefit from medications for much of their life, but it can be a challenge to stick with the medications when all seems well years down the road. Commonly prescribed medications for this disorder include a mood stabilizer (like lithium), while some treatments may also involve the use of additional medications (like an atypical antipsychotic or, in some cases, an antidepressant).
Learn more: Treatment of bipolar disorder
Living With & Managing Bipolar
There are many challenges to living with this condition on a daily basis. What are some of the long-term, successful strategies to staying well, sticking with treatment, and maintaining a balanced mood?
One important component of living with this condition is learning to build routines and sticking with them, no matter what. What can often drive a person into a manic or depressive episode is going off of their routine, or deciding one day that the mood stabilizer that helps them regulation their moods is no longer needed.
These articles were written to help a person learn to live more successfully with this condition:
- Living with Bipolar Disorder
- Building a Successful Routine that Works
- Helping Your Partner Manage Bipolar Disorder
Prognosis
With appropriate treatment, the outlook for someone with bipolar disorder is favorable. Most people respond to a medication and/or combination of medications. Approximately 50 percent of people will respond to lithium alone. An additional 20 to 30 percent will respond to another medication or combination of medications. Ten to 20 percent will have chronic (unresolved) mood symptoms despite treatment. Approximately 10 percent of bipolar patients will be very difficult to treat and have frequent episodes with little response to treatment.
On average, a person is free of symptoms for about five years between the first and second episodes. As time goes on, the interval between episodes may shorten, especially in cases in which treatment is discontinued too soon. It is estimated that a person with bipolar disorder will have an average of eight to nine mood episodes during his or her lifetime.
Getting Help
There are many ways to get started in your journey of recovery from bipolar. Many people start by seeing their physician or family doctor to see if they really might suffer from this disorder. While that’s a good start, you’re encouraged to also consult a mental health specialist right away too. Specialists — like psychologists and psychiatrists — can more reliably diagnose a mental disorder than a family doctor can.
More Resources & Stories: Bipolar Disorder on OC87 Recovery Diaries
References
American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders, Fifth edition. Arlington, VA.
Caponigro, J.M. & Lee, E.H. (2012). Bipolar Disorder: A Guide for the Newly Diagnosed. New Harbinger.
Fink, C. & Kraynak, J. (2015). Bipolar Disorder For Dummies. For Dummies, New York.
Miklowitz, D.J. & Gitlin, M.J. (2015). Clinician’s Guide to Bipolar Disorder. Guilford Press.
National Institute of Mental Health. (2019). Bipolar disorder. Retrieved from https://www.nimh.nih.gov/health/publications/bipolar-disorder/index.shtml on May 22, 2020.

